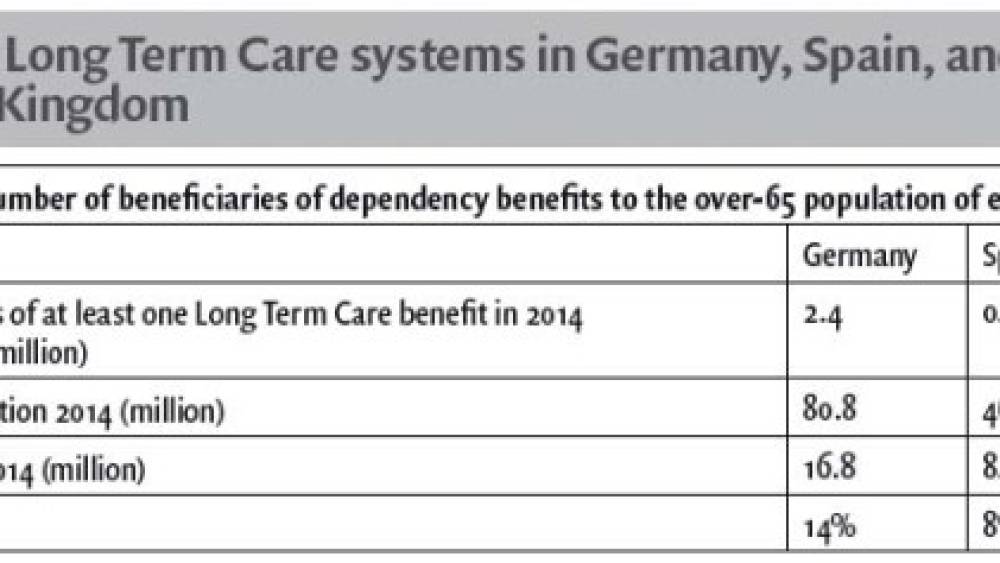
According to the Eurostat report of September 2016, nearly 27 million people aged 80 or over in the European Union. Although their proportion shrank between 2005 and 2015, women still accounted for around two-thirds of elderly people in the EU. This overrepresentation of women among people aged 80 or over is observed in all EU Member States. The ageing of the population structure is, at least partly, the result of an increasing life expectancy, which grew at the age of 80 from 8.4 years in 2004 to 9.5 years in 2014. The subject of financial protection for the elderly is crucial in all countries.
Long term Care coverage in each country is still marked by its past, with a hybrid of Beveridgean and Bismarckian systems, as well as the conservative traditions of some countries, and family traditions of Southern European countries.
- In the Bismarckian model, long term care protection, like any social insurance, depends on labor and social contributions. Insurance helps contributors (and their family) with proportionality of benefits to contributions, and contributions by employees and employers. Versions of this approach are found in Germany. Like most other countries, this model provides a safety net for individuals under the poverty level.
- In countries with Beveridgean tradition, social protection is supported by the national government unrelated to employment and it strives for egalitarianism through uniform benefits. The social protection is financed by taxes. This model is also referred to as ‘social democratic’, and while it is primarily funded by a central government, it decentralizes implementation to municipalities. The Spanish system is also affected by the Beveridgean model.
- Conservative tradition provides greater recourse to the market. But the UK government, as in nearly all countries, has put in place a safety net for the poor. A version of beveridgian system can be found in the UK, where health care is provided through a national tax supported system.
- The family tradition model in Southern Europe has long left Long Term Care responsibilities on families. This collective choice has been progressively challenged with rising female employment rates.
Model 1: Long Term Care coverage principally through public programs
Public Long Term Care coverage is financed either by taxes, as in the Nordic countries, or through social Long Term Care insurance schemes.
The German case
General principle
A 1994 law establishes a mandatory fifth branch, Long Term Care, to the Social Security program. Priority is given to home care over institutional care. The amount paid to disabled people and the frail elderly is fixed (and is not adjusted due to income or assets) but varies depending on the level of disability; whether care is provided at home or in an institution; and whether the beneficiary receives benefits as cash rather than in-kind services. Where charges exceed the allocated amount, the recipient is responsible for the payment of the difference and, if he or she cannot, local social assistance makes up the difference.
Although the majority of Germans fall under the public insurance plan, about 10 % are covered through private insurance, which is compulsory for people who have private health insurance. Supplemental private insurance is also available, and covers about 4 % of the population (some of whom have private, and some of whom have public insurance).
The law covers all forms of loss of autonomy, regardless of age. Since January 2013 it distinguishes four levels of dependency, according to which services (personal care, home care) are needed. Beneficiaries of public funds may choose between benefits in kind, delivered at home or nursing facilities, and cash benefits, or may take a combination of the two. To be entitled to Long Term Care insurance benefits, applicants must have been insured for at least two years. However, insureds through a private fund may collect indemnity benefits for specific services.
The four disability levels are:
- Level 0: people who, because of dementia, a mental disability, or psychological disorder, are severely limited in the exercise of Activities of Daily Living, without the level of aid needed for a person described in Level I;
- Level I: those in need of care at least once a day for bodily care, feeding, and mobility;
- Level II: people whose dependence is heavy and need help at least three times a day for basic care and at different time of the day;
- Level III: those whose dependence is absolute and permanent and need help 24/7.
In addition, Long Term Care funds support the costs of specialized equipment (a hospital bed, for example) and costs related to home modifications, subject to a deductible. Two thirds of beneficiaries opt for cash payment and live at home. Of these, one third receives care from private operators, while others are assisted by a family caregiver paid in part through Long Term Care insurance.
Financing
Compulsory Long Term Care insurance is backed by the health insurance Social Security program. Thus, any person affiliated with the national health plan or with a private insurance plan is automatically affiliated with his or her Social Security health insurance coverage.
The Long Term Care branch is funded by a payroll tax rate of 2.05 % (as of January 2013) shared equally between employees and employers. To compensate the employer's share, a holiday was removed in 1995. People who do not have children pay an additional contribution (0.25 %) and retirees participate in the financing of Long Term Care Insurance by paying a contribution proportional to their assets. Financing of social services is provided by the municipalities.
Model 2: Long Term Care coverage combined with the subsidiarity principle
The second model includes the so-called "hybrid system" with several elements supporting a basic income. Spain uses this hybrid system. Benefits are usually capped. Public financing complements the revenues and assets of the dependent elderly.
The Spanish case
General principle
The 2006 Law No 39 on the promotion of personal autonomy and care for dependent persons provides for the progressive implementation, starting on January 1, 2007, of a national Long Term Care apparatus which covers all forms of dependence irrespective of causes (age, illness, etc.). Under section 33 of the law, the amount of aid is determined according to the resources of the beneficiary.
The law defines three stages of dependence and subdivides each into two levels. It also determines the list of benefits in kind (from technical devices facilitating home stay to residency in a specialized establishment) which are proposed to the dependent by local social services and, if unavailable, by accredited private providers. The law favors in-kind services over cash, which is granted only if direct services cannot be provided.
The System for Autonomy and Attention to Dependence (SAAD) expands and supplements the public program by providing prevention services or reimbursement for services.
The benefit is most often used to pay for home care: 1.4 million people, including a large majority of women (77 %), live alone. But this service is also used to cover the costs of accommodation in a specialized institution. Benefits are adjusted based on the beneficiary’s income, such that some participants must pay up to 90 % of the cost of home care and up to 65 % for other services.
Financing
Financially, the law provides for the cooperation of national and local governments, with financing by local governments to be at least equal to the national government’s share. National contributions are divided into two parts: first a contribution for the dependent person and also an amount negotiated with local authorities. Furthermore, beneficiaries participate in the financing of the program according to their ability to pay (income and assets).
Model 3: Long Term Care coverage based on social assistance
The third model is that of a means-tested minimum safety net. The OECD places UK under this model. The following description applies mainly to England as benefits differ in other regions. Scotland, for instance, provides free personal care.
The British base (England)
General principle
The 1990 Law on the National Health Service and Community Care Act makes a clear distinction between health care, which is the responsibility of the National Health Service, and Long Term Services and Supports, which are part of the social care system, and entrusted to local authorities.
Individuals 65 or over who need Long Term Care can receive the benefit of assistance called “Attendance Allowance”. The amount of this benefit depends on the degree of dependency and is not subject to means testing. In 2013 the weekly benefit was ₤53 or
Local authorities may support some Long Term Care costs based on a person’s needs as well as resources, including their home. Local services must plan and manage how services are provided, but do not have the obligation to provide them directly: they can use private providers or can reimburse the beneficiary for the needed services.
For expenses associated with nursing homes in general, costs are fully borne by persons whose assets exceed ₤26,500 (in 2013). Below ₤26,500 of assets, the amount of aid corresponds to the difference between the price charged by the nursing home and the income of the elderly, plus ₤1 of copay for every ₤250 of assets.
Financing
Funding is provided by the national government through tax.
An heterogeneous system
Long Term Care policies vary widely in Europe. The only regulations that deal with the issue are about coordination of programs:
- A regulation coordinating social security systems. Long Term Care cash benefits are exportable, but not benefits in kind, when an insured person changes member country residency;
- A regulation on the mobility of patients mentions Long Term Care, only for the exclusion to the scope of its regulation. This exclusion is an important part of the political compromise that has prevailed.
Points of convergence
- Priority of home care, which meets the demands of the inhabitants and involves, for most early programs, a break with "the very institutional" 1970;
- Development of cash benefits instead of benefits in kind, in the form of allocation of hours services. This allows better control by the financing entity (national government, local government, and social security) and greater flexibility of use by the beneficiaries, especially for caregivers;
- A trend toward free choice of providers, even for benefits in kind granted under the auspices of public authorities;
- A limited role for private insurance. The role of private insurance is generally small and weak in terms of population covered (See Box).
Diversity of funding
When analyzing Long Term Care financing more generally, regardless of payer, it appears that in most countries, financing is diversified, involving all resources: national and local taxes, social security, and private sources whether through the beneficiary's resources or private insurance.
Private funding is significant in Germany and in Spain where benefits follow a fixed guideline. Private funding is low in the Nordic countries where the ceiling for households’ participation and a minimum benefit for the “remaining life expectancy” protect the poor, both at home and in institutions.
Expense projections
Public expenditure management of Long Term Care in 2010 averaged about 1.5 % of GDP in OECD countries, excluding institutional residence expenses. Projections give a very significant increase in these costs by 2050. The baseline average for OECD countries, should reach 2.4 %.
A variety of definitions
Apart from the purely financial aspect, which will be a major challenge in the coming years, we should, for better convergence, achieve a shared set of definitions for Long Term Care and its measurement, for example:
A distinction of functional dependency and cognitive impairment, because with the exception of France and the UK that mandate an age requirement, other countries aggregate physical and mental disability, or criteria for "duration and care" and "care utilization" to accomplish Activities of Daily Living.
A convergence is rendered more difficult as benefit measurement depends not only on the level of dependency but on the nature of service and the delivery system. In Sweden, for example, Long Term Care is supplied not according to the concept of dependency, but according to one’s needs;
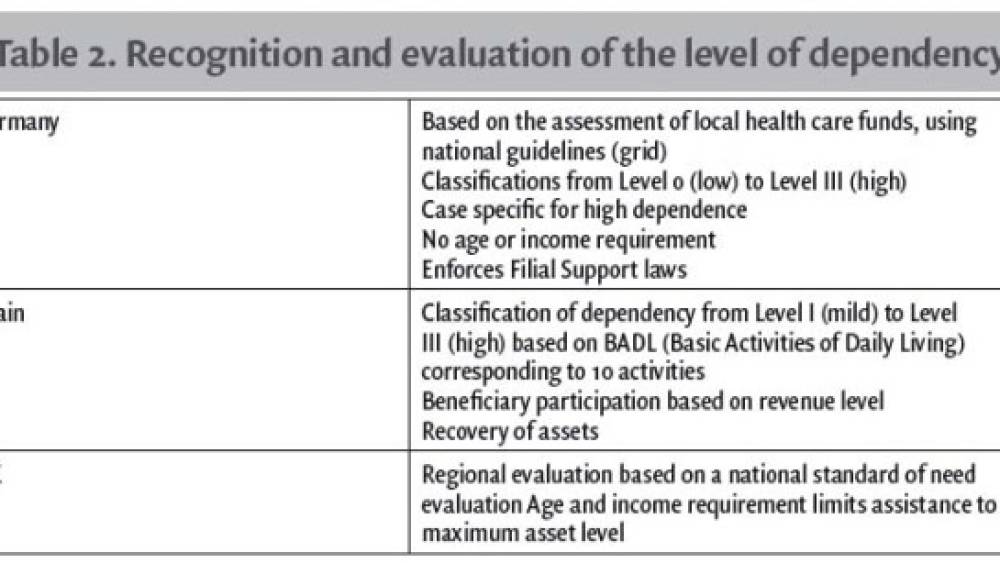
The recognition and evaluation of the level of dependency differs by country (See Table 2).
xxxtable2xxx
Conclusions
Foreign examples help us think about the best ways to cover public and private LTC expenditure. Insurers have an indispensable role to play in the solvency of the insured person beyond public aid. The regime of tax and social benefits should support the insurance offer, savings or pension, collective or individual contract, main or supplementary, as planned in France the law on the adaptation of society to aging. Help for caregivers is a major focus of the insurance offer. A multitude of services or innovation (connected objects) seems to have no limits.